Saying Goodbye To The Kojo Nnamdi Show
On this last episode, we look back on 23 years of joyous, difficult and always informative conversation.
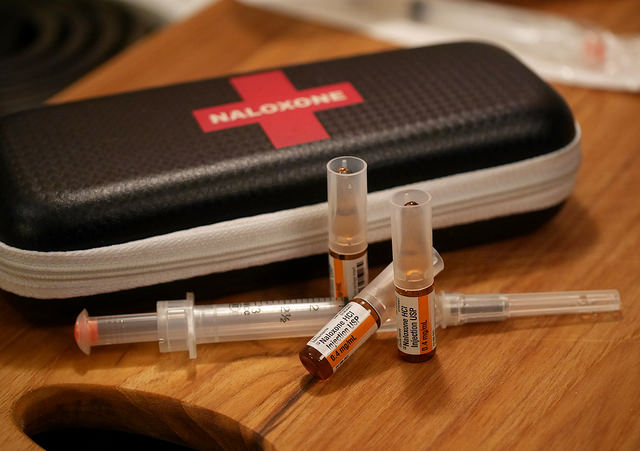
Naloxone kits can be life-saving for those in danger of opioid overdose.
The opioid epidemic is often painted as a crisis plaguing rural towns and suburbs. But in Washington D.C., African Americans die of overdoses at a higher rate than whites in West Virginia, Ohio or New Hampshire.
A Washington Post investigation revealed just how severe — and neglected — the epidemic is. Last year, more District residents died of opioids than homicides. And the response from local government agencies has been lacking…until now.
A strategic plan released by D.C. government at the end of December promises to cut opioid-related deaths in half by 2020. But what does that plan entail? And how much damage has already been done?
Produced by Julie Depenbrock
KOJO NNAMDIYou're listening to The Kojo Nnamdi Show. I'm Dan Reed, sitting in for Kojo. Every time we've discussed the local impact of the government shutdown, our phones have been flooded with callers. We haven't been able to get everyone on air, but some of you sent messages to kojo@wamu.org on the shutdown's more under reported effects. Let's take a listen.
BOBMy name is Bob LaGrand, and I'm a retired federal employee, but at one time I was a loan executive to the combined federal campaign a number of years ago. It occurs to me that since the campaign ends next week that -- and a lot of people wait to do their pledges until the end that a lot of charities in the national capital area are going to be hurting, because they don't get the pledges that they would have gotten if the government were open.
ANNHello, this is Ann from Bethesda. I am an NPS biologist who is not hiring interns for the summer employment. I should be hiring PhDs for post-doc work. I should be hiring people getting their master's degrees. I should be interviewing undergraduates getting ready to enter the job market and hiring them to provide NPS managers with materials to protect natural resources in our national parks. And that is not being done.
ALEXMy name is Alex. I'm from Alexandria, Virginia. I'm one of the lucky ones where I can still make ends meet even if I miss a pay check or two. But the shutdown and the uncertainty that's come with it has led me to make some changes. For example, I was planning on buying my first home during the first few months of the year, but I'm not longer even considering that because I can't make true financial decisions in the short and we don't know when this is going to end. And it will have repercussions for the long term, as well.
UNIDENTIFIEDHi, Kojo, so far I haven't heard any one report on the impact the shutdown is having on families with children at federal daycares. My husband is at DOD, which isn't shutdown. I'm not a federal worker. My daughter is at a daycare at an agency that is shutdown, where we have to keep paying the daycare bill. In the meantime, we don't have child care. This has put a strain in our family financially and psychologically as we try to jungle jobs and securing reliable alternative care for our toddler.
DAN REEDYou can still send us your 30 second story at kojo@wamu.org with the subject line shutdown. Now on to the rest of our program, the opioid epidemic is often painted as a crisis plaguing rural towns and suburbs. But in Washington D.C. African Americans die of overdoses at a higher rate than whites in West Virginia, Ohio, or New Hampshire. And it's hitting a surprising demographic, older African Americans.
DAN REEDLast year more district residents died of opioids than homicides. And the response from local government agencies hasn't kept up with the scale of the crisis. A strategic plan released by D.C. government at the end of December aims to cut opioid related deaths in half by 2020. What does that plan entail and how much damage has already been done? Joining us to discuss today is Peter Jamison, a reporter with The Washington Post. Thank you for being here.
PETER JAMISONHappy to join you.
REEDPeter, we've heard a lot about the opioid epidemic around our region and the country, but you say it looks very different in D.C. from the crisis unfolding elsewhere. What did you discover in your reporting?
JAMISONIt does look very different. And when we read and hear about the opioid epidemic in 2018, now 2019, many people associate it with a rural, sometimes suburban phenomenon, often afflicting younger users. Many of whom are originally addicted to prescription pills and then moved on to heroin. And, you know, there's been a lot of coverage of the resurgence of heroin in recent years.
JAMISONIn D.C. what you have is a very different phenomenon. You have a population of long term chronic heroin users, who have been using for, you know, 20-30, in some cases, no kidding, 40 or 50 years. These are people who first became addicted to heroin when it really began taking over American cities on the east coast and the mid-Atlantic in the 1960s and the 1970s who have continued to use since them with something resembling functional addiction. You know, often they'll keep up a job of some kind, maybe a fairly menial job, but some kind of work and they have been able to hone their habit over time to the point where they can use relatively safely.
JAMISONBut all that changes when you in 2014 and 2015 see the entry of the synthetic opioid fentanyl into the heroin supply in the United States. And what does --fentanyl is synthetic opioid that for a half century was used for patients in very chronic intense pain, sometimes as a surgical anesthetic. Beginning in -- and people quibble over the dates, but sometime in 2014 or 2015 it began to be mixed into the U.S. heroin supply.
JAMISONThere's a lot we don't know about fentanyl, but the general consensus is that much of it is manufactured in China. It comes into the U.S. through Mexico and is mixed into heroin here. And when that happens fentanyl is such a potent drug that even slight miscalculations, when you mix it into heroin can be deadly.
JAMISONSo you've got this group of users that have been using a substance for literally decades. And they think they know how to use it. And then over night that substance changes in the way that makes it deadly and they can't use it safely anymore and they begin dying. And that's really what we've seen here in the District and in other American cities as well in the last few years.
REEDIt was The Post's recent investigation into the opioid crisis in Washington that revealed just how severe and neglected the opioid epidemic is among this population.
UNIDENTIFIED SPEAKERI've wasted so much time, so many years of my life. I've missed out on my kids' life and up to now the drugs are still in the way and still very much a part of my life. I'm like really been doing this close to 30 years, My God.
REEDWhat you just heard was an excerpt from a video by The Washington Post's Whitney Shefte. Peter, you found the opioid epidemic among this population in particular, older African Americans, has been largely overlooked amid all of the coverage of the crisis. And that it's not typical of the epidemic elsewhere. What did you find?
JAMISONThat's right. So once again, there's been a lot of coverage of fentanyl entering the U.S. drug supply. What there's been comparably little attention to -- and I don't want to say there's been no attention to it, because there have been some, you know, non-profits, think tanks, some journalists who have brought attention to this. But it's received far far less attention than other aspects of the epidemic.
JAMISONBut there is this new kind of sub-plot to the opioid story, which is that there's been an extraordinary surge in deaths among African Americans in large cities. And this is borne out by data we looked at from the Centers for Disease Control and Prevention. You know, last year 7 in 10 African Americans who died of opioid overdoses lived in a county that was categorized as heavily urban by the National Center for Health Statistics. That's compared to 3 in 10 whites. So what we see here is an urban predominantly African American phenomenon where deaths are skyrocketing.
JAMISONAnd until 2015 -- 2014 and 2015 the rate of fatal drug overdose among African Americans as, you know, this opioid epidemic has been consuming the country rose comparably slowly compared to whites. Since then the rate of fatal drug overdose among African Americans has increased more than twice as fast.
JAMISONSo fentanyl has decimated opioid users of every demographic and I don't want to imply that it hasn't. In rural places, suburban places, you know, big cities, but the effect has just been extremely pronounced among this population of chronic users, who again because they're using heroin and thought they could use it safely were particularly hit hard and sort of caught off guard by this new development.
REEDWe've got a call from James in Silver Spring, Maryland. James, are you there?
JAMESYes.
REEDThanks for calling.
JAMESI'd like to ask the guests and you why we rarely if ever hear anything about how the war on drugs makes the epidemic worse and actually increases the harm of drug use. I did hear someone say that, you know, when you buy -- you have adulterated products -- and that's one of the effects of the war on drugs. If you buy on a black market, you don't really know what you're getting. Whereas if it was regulated market for these where you had medical personnel and also there's the stigma of, you know, it being illegal. So we really have more discussion about how the war on drugs makes this worse.
REEDThank you. Also joining me here today are Edwin Chapman, an Internal Medicine Specialist in Washington D.C., who's been practicing for 41 years. Thanks for being here.
EDWIN CHAPMANThank you.
REEDAnd Diane Jones, Director of Special Programs and Field Education with Family and Medical Counseling Services in D.C., which has been on the front lines of this crisis. Thank you for being here.
DIANE JONESThank you.
REEDWhat do you all think of what this caller just asked?
CHAPMANWell, for my perspective as an internist practicing in Washington for the past 41 years and substance abuse for the past 19 years, we began to look at substance abuse as a chronic disease. You must remember that we had very little training in substance abuse in medical school generally. And it's only been three years since substance abuse was considered a specialty.
CHAPMANSo as of 2016 or so, it actually became a bonafide specialty. And that's important because until that time substance abuse was looked upon as a moral problem, so all of our approaches were treating a moral problem as opposed to a medical problem. And that has a great significance going forward. So we're still in that transition period where there are many people who still perceive this as a moral problem as opposed to a medical problem.
REEDHow do you treat someone who's addicted to opioids?
CHAPMANSo opioids are very different from any other addiction. It mimics the body's feel good system. We have chemicals in our nervous system called the dopamine system that make us feel good. So when we wake up in the morning and you get a cup of coffee or something great to eat, it makes you feel good. Opioids highjack that system and they're very different from cocaine or tobacco or alcohol in that this really comes as close to that system as possible. So what we found is that without medication assisted treatment there's a 90 percent relapse rate in this particular disease. So that medication is the gold standard along with counseling at this point.
REEDDiane, you've been overseeing the Needle Exchange Program at Family Medical Counseling Services now since 2008. What population do you serve and what changes have you seen in the past decade?
JONESThank you. First I want to say thank you to the medical examiner's report because that seminal report, actually got us here and shed light on the deaths that we're actually seeing in D.C. We service a older African American population of substance users. And that's been our population even before 2008 with our out-patient substance abuse treatment programs. However, with the fentanyl poisoning going on the District, we've had to take other measures (unintelligible) reduction programs and use prevention measures that would have combat some of this, which is the Narcan as one of our tools in preventing the overdose.
REEDYou've said that on a monthly basis you're running out of the lifesaving drug Naloxone. How do you tell someone, who's in danger of an overdose, that you don't have the antidote?
JONESGood question. So it varies day to day. There's no good answer. I mean, that's the five million dollar question. Any answer is going to be a five cent answer. But we ask in our team every day. Since October, we've been able to purchase our own supply of Narcan. But before then we ran out on a monthly basis. So at any given point we have about three to four sites that we do daily in the city. And so you might have five kits for that site. So you have to tell those other 15 people that you don't have any more Narcan. And so that's a decision, daily that people have to wrestle with and discern, who's the person to give this to. There is no easy way. There's no way to discern it. You just hope the next day you didn't hear about that person overdosing.
REEDWe'll continue our conversation after a short break. Stay tuned.
REEDWelcome back. I'm Dan Reed in for Kojo Nnamdi. We're talking about the opioid crisis in D.C. Got a phone call from Tony in D.C. Tony, you're on the line.
TONYWhy thank you very much. You know, I think that we are at a very unique time in the District of Columbia. You know, we're in the middle of a huge gentrification that's also impacting I think many major cities. The opioid crisis that we see happening in rural American is also happening in urban communities. And one of the challenges is how do we address it in black populations versus how we're treating it in white America.
TONYAnd I think the reporter has done an amazing job. We saw that Candace Montague did an amazing report in the City Paper talking about the opioid crisis in older African American communities. But I think one of the pieces that we miss often is getting actual people who inject drugs and use drugs and have used drugs for decades involved in developing policies.
TONYBeing those people that are out there with Narcan supplies, who can prevent overdoses and really preventing both deaths, but also preventing overdoses and making sure that we're having a conversation about preventing overdose and preventing deaths, but giving people who use drugs the opportunity to set policy and to also be able to prevent overdose within their community and their social networks, their drug using networks and within their community.
REEDThank you very much, Tony. So I want to ask our guests, you know, you heard some the issues that Tony is raising around this crisis in D.C. You know, what kind of effect does the opioid crisis have on this community?
CHAPMANIt's -- I call it a tsunami. We look at the individual, but we forget that each one of these patients that dies impacts folks around them. Their family, the community and so every time we have a death it has a -- it just grows. It's a chronic disease that creates other chronic diseases. So there's crime associated with it. You have infectious diseases associated with it. Family is impacted. Economics are impacted. So that we've identified at least seven or eight other chronic problems associated with -- child welfare costs go up. So it has a tremendous ripple effect throughout the community.
JONESAnd I think we can't afford to whitewash this issue in the District any longer. I think that the coroner's report showed us the number of deaths. Before that, this population was invisible. It became visible with those numbers. We can no longer deny that people were dying. And this same population was ignored through the crack epidemic.
JONESSo it's the older community who've been using for years. We need a different approach. And our approach is one on one. They don't respond to this approach we've been doing. We need a one on one grassroots level -- community based level approach to this population and we need resources. So if somebody dies or overdoses in your house, you didn't lose your housing. We already have no affordable housing. So this complicates the issue even further. So people appear overdosing in my house, I'm going to drag you out into the alley to die, because I don't want the police at my door.
REEDDiane, you've worked with individuals affected by the opioid crisis for over a decade. And you say that D.C.'s government agencies have been slow to respond to this crisis. What do you think the obstacles have been?
JONESI think collaboration. I think we have not collaborated. Everybody has been working in their own silo. We have not kept pace with demographics. We have not kept pace with the changes that have been happening with the epidemic. So it's going to take all of us, the government, academia, community based levels, medical providers, to come together to respond to this. No one entity can do it alone. So I think our lack of collaboration has caused us to be behind.
REEDWe're also here today with Roger Mitchell. He's the Chief Medical Examiner for the District of Columbia. Thank you for being here.
RODGER MITCHELLIt's my pleasure.
REEDYou know, Roger, a lot of local governments have been struggling with these epidemics that came up fast and overwhelmed their agencies. This is not unique to the District of Columbia. How would you say D.C. has responded to the increase in fatal overdoses?
MITCHELLWell, let's put it in perspective. I think that we heard how these death occurred and the numbers, but in 2014, we had about 80 to 90 opioid overdose related death in the District of Columbia. And in 2017, we had 279 opioid related deaths in the District. So -- and again, largely black men, 40 to 60, but the concentration between 50 and 60. And so, those early years really trying to understand I think the government in 2014 and 2015 really trying to get a handle on whether or not this was an upward trend that we were dealing with.
MITCHELLIn 2015, Mayor Bowser established through the Department of Health and the Department of Behavioral Health a opioid task force that started back in 2015, interagency governmental type of work group that started monitoring and looking at the data surrounding these deaths. Fire and EMS is at the table, law enforcement, the medical examiner, the Department of Health, Department of Behavioral Health in 2015.
MITCHELLAnd then over 2016 and 2017 really trying to get an idea of how the government should respond. In 2017, they convened about 40, we convened about 40 stake holders. All of this is included in the "Live Long D.C." report that is really the culmination of the work that has happened between 2015 and now to prepare the government to respond in even a better way to the opioid overdoses that we're seeing.
MITCHELLAnd so now we're culminating with $23 million that's available through federal moneys and people at the table from all agencies as well as all parts of the community that's looking at this issue, hoping to cut these deaths by 50 percent by 2020, which is a very aggressive approach. But I think your other panelists, colleagues that I have here on this panel, realize how important it is to now work with haste to save lives in this epidemic.
REEDWe've got another call from Max in D.C. Max, thank you for calling.
MAXThank you for having me. I was calling. I really do not feel that this is a disease. I think this has to do with weaknesses among the people, who are abusing it. I have been prescribed opioids after dental and other types of surgeries. I take either some or most of them as it was needed. And then it's done. You know, I don't continue using it and abusing it. And not everybody does that.
MAXSomeone abusing a drug doesn't make it a disease and the woman who was speaking earlier when you were talking about shortages of Narcan and some other things. I think someone mentioned you know someone in jeopardy of overdosing. Well, don't take it. Don't use it in the first place, you won't be in jeopardy of overdosing. You know, this has to do with people's weaknesses. I think that we're just making it easy for people to continue to overtake and die by treating it like a disease rather than treating it like--
REEDThank you very much. Max, thanks for calling. I've got a lot of reactions here in the room. Edwin, you are a doctor. What is the difference between somebody taking this for pain and becoming addicted to it?
CHAPMANSo we know much more now than 40 years ago, when I was in medical school, about how these medications work. But most medications are metabolized through the liver. It's called cytochrome P450 system and there are about five different pathways. And what we know now are that different people depending on your genetics metabolize drugs differently.
CHAPMANI for one happen to be allergic to morphine. So that tells you if I'm allergic to morphine and somebody else takes a morphine like medication and it makes them feel good, then there's a difference in the way our bodies handle that. So now we're able with genetic profiles to start looking at that. And I'll just give you a quick example. Codeine, which is commonly put in cough syrup given to children, etcetera, was found about six years ago that about 20 percent of the population of what we call ultra-rapid metabolizers -- and children could actually overdose over with a typical cough syrup. So now the labeling has been changed. So that's just one example of an opioid.
CHAPMANNow we have all of these different opioids, oxycodone, Ultram, fentanyl, and this street fentanyl that has all of these different analogs that we have no idea what's in them are metabolized differently. Give you another example. I have a whole group of patients probably 20 or 30 patients that test positive for fentanyl on a weekly basis and never overdose. So they must be rapid metabolizers of fentanyl. So I think that's part of the underlying problem with the justice system and with the whole stigma system is that everybody thinks that they're like me. We're all different.
REEDAnd, Roger, how are these people different? How does one get addicted?
ROGER MITCHELLWell, I mean, it's really good and, you know, just for a full disclosure, I'm a physician, as well, a forensic pathologist. And to put it in perspective for the listeners, when someone has trouble breaking a habit of smoking, smoking is an addiction. And so someone may suggest that that smoking addiction is some weakness in that individual for smoking. But the reality of it is is that they're smoking, and once they get addicted, is because of the nicotinic receptors as other receptors that are responding to what's in cigarettes that makes them addicted. The outcome of cigarette smoking is well known. It's cardiovascular disease, or tumor or cancer of the lung.
ROGER MITCHELLWe would never look at a patient that is suffering from cancer or cardiovascular disease and tell them they have moral failures. The outcome of drug addiction tends to be having moral implications, because of that high-jacking of the pleasure centers that Dr. Chapman spoke about. So, that addiction and really going upstream for the addiction is filling an emptiness that needs to be filled, particularly in communities of color that we're talking about, communities that have a history of institutional racism, have a history of lack of access. These are the types of things that would lend anyone to drug addiction.
ROGER MITCHELLAnd so when we see drug addiction in the rest of the world -- I mean, the rest of this country, it is largely in the Appalachians and other parts of West Virginia and other parts of Ohio that have access issues. They tend to be white, young people, but some of those same issues. So, we're not just talking about those that have gotten addicted because of their pain medications. We're talking about those that have had some issue outside of that that lends them to utilizing the drug. They have some addiction, then, and then those are the outcomes of addiction. So, when we think about addiction, you have to think of it as a disease, because it's both preventable and it's treatable. And so, as physicians, something that is both preventable and treatable is uniformly called a disease.
REEDAnd, Roger, I understand that your family has had some personal experience with addiction, as well. Could you talk to that a little bit?
MITCHELLAbsolutely. So, I grew up with a crack cocaine-addicted father. And so, I'm an X-gen. So, those of us that were born in the '70s and were raised in the '80s often had, that because that's when the crack cocaine epidemic was hitting our communities. And I came from, and come from, a, you know, middle to upper-middle-class family. My father was an entrepreneur. You know, my mother was a professional. And so the addiction came at a time of depression for my father, when he lost his mother, and caught him, and he was addicted for many years. And then I grew up, and we talk about the tsunami. I grew up fatherless in a space where I was able to connect with other men in my space in the form of my grandfather, who was a physician, to give me the hope to be able to move beyond that.
MITCHELLThe point that I'm making is is that drug addiction can and does affect all communities. Today, we're talking about an opioid crisis that has been largely shown as a young, white problem in the rural and suburbs of this country. And what we're doing well here is discussing that this is an issue that is also affecting urban communities, particularly Washington, D.C., disparately within these communities. And we've set out a roadmap. We've set out a roadmap in the form of Live Long D.C. We set out a roadmap in the form of Working with Partners in order to move towards life safety, because it's a disease, and not a moral failure.
MITCHELLMy father now is clean. He's been clean for 10 years. He's a substance abuse counselor, and he's good at it. It's awesome. And so peer-to-peer, you'll hear this peer-to-peer, and it was said before, the grassroots construct surrounding peer-to-peer and making it relevant for people that have been able to get over the drug addiction is really powerful to help other people kick the habit and recover from this chronic disease.
REEDI wanted to shift to talking about some of the potential solutions that there are. You know, Roger, you've alluded to the city's plan to address opioid issues. We've also got a call from Phil in Frederick. Phil, are you there?
PHILYes, I am, sir.
REEDThank you for calling.
PHILThank you for taking my call. I've got a pretty elaborate first-aid kit, and I'd like to know where I can get lessons or information about first aid for the use of NARCAN and the means of saving somebody's life in the event.
REEDThank you very much, Phil. (laugh) Any thoughts?
JONESSo, in most health departments, I know in the state of Maryland, the health departments are offering daily trainings in Naloxone, as well as giving kits. And that's in the state of Maryland.
MITCHELLI would have the caller, and I just forgot his name, he can reach out to D.C. Health and see what D.C. Health has available, as well as D.C. Department of Behavior Health, as to see what we have available in the city for that type of training.
REEDWe've got another call from a public health worker. Barry in Garrett Park, Maryland, are you there?
BARRYYes. Yes, I am.
REEDThanks for calling.
BARRYMy concern is that a lot of people who are using drugs don't have any way of knowing whether there's fentanyl in the drugs, and that that's probably a major cause of death from drug overdoses of people who had no intention of killing themselves. And so I think that the public health question is, how come these tests for fentanyl, which I understand are technically available, are not made more widely available in rehab and practiced on the street so that people can see what they're using and avoid something that's got a lot of fentanyl in it?
REEDThank you very much.
JONESSo, good question. And so we have what we use called fentanyl strips. They're very expensive, but we are able to purchase some and give the people that they can test their package to see if there's fentanyl in their package. So, it does exist, not on a wide sale yet, but hopefully with some of the additional funding coming, we'll be able to purchase more of those strips.
REEDHow expensive is this?
JONESThey're a dollar a strip.
REEDHum.
MITCHELLAnd so, as part of this plan that is Live Long D.C., part of the initiatives in the harm reduction category goal is the fentanyl testing strips. And so there's a considerable amount of money that is going into each one of the goals to be able to achieve them. And part of that is making these strips more widely available.
REEDNow, Peter, you're a reporter for the Washington Post. You've covered this issue for many years. And you and other reporters have been fairly critical of the way the D.C. government has handled this spike in overdoses. What do you think of the strategic plan that D.C. has put forward to deal with the crisis?
JAMISONI think the most important thing to realize about the strategic plan is that it's a plan. It's a piece of paper. It's two dozen pages long. It's the product of a lot of extremely competent and well-meaning people who have worked on this over the course of the year. But, you know, for anyone who's followed the D.C. government's response to this crisis, you can't look at this plan and not recognize a lot of things in it that the city's either, A., already doing or, B., was supposed to be already doing. I'll give you an example.
JAMISONYou know, one of the goals here is to ensure timely access to substance abuse disorder services in emergency rooms and hospitals. This is something that's happening in many part of the country. There is a landmark 2015 study at Yale New Haven Hospital that showed that opioid overdose patients who come into the emergency room, if they're started on one of the medications that Dr. Chapman mentioned earlier that diminish cravings for opioids -- this particular medication is called buprenorphine, often prescribed under the brand name Suboxone. If they're prescribed that in the emergency room, they have a much greater success rate long term in staying with their treatment.
JAMISONA program of this nature was supposed to be set up at D.C.'s public hospital, United Medical Center in Southeast, which last year saw 400 opioid overdose patients, far more than any other in the city. And it basically just never got off the ground. And Dr. Chapman, I know, can speak about this a little bit, because it was his organization that was supposed to partner with the city on it. But, you know, you had a situation where a medical provider arrived at the hospital in anticipation of creating a program like this for patients. This is a situation, again, where, I mean, hundreds of people would've gotten counseling and outreach services that just did not get it.
JAMISONAnd what happened was the city had told the federal government that they were going to use federal funds that they received in the amount of $4 million over two years, in part to establish this program at United Medical Center. Again, this is a proven intervention that is known to be effective. And while the private partner in the effort, Dr. Chapman's practice, did their part, the city did not do its part. It did not establish any outreach workers there to kind of facilitate the program.
JAMISONSo, while this sounds like a normal bureaucratic failing, there're very real consequences for this. One of the gentlemen I spoke to in my stories was named Philip Williams. His brother is named Victor Williams. He's an opioid user of the demographic we've been talking about here today. He had used for decades. He was treated at United Medical Center for an opioid overdose. He was released. On the day that he was released, he died from another opioid overdose.
JAMISONAnd this is someone who, while, you know, you can't say he definitely would've been helped, he definitely would've gotten treatment, because each -- you know, you can't force anyone into drug treatment. There is a level of individual choice and responsibility behind each of these patients. But he at least would've had a better chance than what he did have, which was nothing. He was let back out on the street, and he died. And, you know, it's impossible to know how many, you know, dozens or hundreds of people like that had similar stories just by virtue of the D.C. government not carrying out a program, which it said, in written documents to the federal government, it would carry out.
REEDI'm Dan Reed, in for Kojo Nnamdi. We'll continue our conversation after a short break. Stay tuned.
REEDWelcome back. I'm Dan Reed, in for Kojo Nnamdi. We're talking about the opioid crisis in Washington, D.C. First, I'd like to go to the phones. Lisa, in Upper Marlboro, are you there?
LISAYes, I'm here.
REEDThank you for calling.
LISAThank you. So, (clears throat), excuse me, I've been listening to you, you know, the callers and, you know, the doctors. And I wanted to share my experience. My son, who's now 30, um, was exposed to oxycodone when he was about 12 years old. He had broken his leg playing around, as kids do, and he was given, you know, a two-week prescription which, you know, you don't -- I wasn't aware of the dangers of the drug. So, you know, every day, I was, Trevor, make sure -- oh, I'm sorry, you take your medication. And he ended up becoming addicted.
LISAAnd then I found out through this process -- you now, we went through a long, drawn-out process. You know, smart kid, one of the smartest people I've ever known, and I couldn't understand where this addiction was coming from. And one of your speakers mentioned that, you know, therapy and medication or the protocol for treatment. And that's what we have found that that is the best protocol. But we also learned through therapy that there had been, you know, some abuse in the past, which I wasn't aware of, and was able to address through the therapy. So, one of your callers mentioned it was a moral, you know, failing for folks who are addicted. And I did a lot of research, because I couldn't understand, you know, why is this brilliant kid, you know, addicted and, you know, not able to just stop.
LISAAnd, you know, you talk a lot about the, you know, the addiction process, but I think a lot of people don't understand, and a lot of people, I believe, once they understand -- especially family members -- then you're able to deal with the addict, you know, in a more effective way, because you understand what they're going through. You understand that there's not a whole lot of control that they have, but, you know, with help and support -- and, unfortunately, it's not a one-and-done. It's a lifetime journey, and you just are basically supporting, you know, that person and understanding what's going on with them.
REED(overlapping) Thank you very much, Lisa.
CHAPMANAnd I think that's why this conversation is so powerful. And if you listen to what Dr. Mitchell said early on, Dr. Mitchell wrote a book called "The Price of Freedom," and I'm not here to plug his book. But I read the book and was just blown away, because how could an eight- or nine- or 10-year-old kid be so far ahead in his thinking in navigating the system? But you must read the book, and I meant to bring four copies or five copies here to give away, because it really shows the complexity of this whole process.
CHAPMANSo, there's a mental health component to substance abuse or any kind of abuse. Forty to 50 percent of patients who become opioid addicted suffer from depression or anxiety, and then it goes up from there. So, you have to add these various components. We're all different. We all have different responses to -- or different levels of dopamine genetically in our system, and we know that now, that we didn't know before. So, depending on where you start, if you start with a low level of dopamine and you're in a high-stress environment, then you're likely to fall into some type of addiction earlier in life.
CHAPMANSome of us are more fortunate and have the support systems, and some of us don't have the support system. But you must really look at this as an individual process in the fact that there are mental health and environmental components that we call toxic stress that play into this.
JONESDan, so I think the caller identified an ideal response and approach to this issue. However, my clientele has been -- unfortunately, racism kind of has kept my clientele from being prescribed those opioids. Because if my clients went to the doctor with pain, they're not getting opioids, because it's already assumed that they're a drug user and they're an addict, and so they're not given that. And so some of the moral treatment of this or the relation to it has caused my clients to go underground and to go to the street drugs for any pain that they might have.
JONESWe're not even going to talk about the health disparities that exists among the population, the HIV and the hepatitis. We're not even going to get to that, but what drives people to use, that we see, is some of the stuff Dr. Mitchell talked about earlier with the hopelessness and helplessness, the no housing, just being poor and no access, and being invisible. And so, finally, we get some light on the issue, because the rest of America was suffering. And so now, here we are, hopefully we can get some resources that will allow people to be healthier, to go to mental health without -- they don't go because of the shame, and people make them feel so bad when they show up to these institutions.
JONESWe have a nurse on our mobile unit that helps people treat their abscesses and their wound care, because when they go to the ER, with the smelly abscess of the wounds, they're turned away. It makes them feel so bad, that they never return. And so they just keep going and lose legs and other limbs because of their shame of what their disease has caused them.
JAMISONYeah, to piggyback on what Diane is saying, I think that, you know, there has been an undeniable change, while it's not complete, as we heard, I think, from one of the callers early on. But there has been an undeniable change in attitudes towards drug addiction in this country, with the opioid epidemic. And, you know, one of the many ways that this epidemic is changing our society is that people have come to view drug addiction as a disease. By and large, they're recognizing that there are effective medically based treatments for it. And there's a level of sympathy for drug users that was simply not present 10 or 20 years ago.
JAMISONBut when you look at this in the context, a bigger half-century-long context, which is what the time frame that the people were talking about here today are looking at this and, you know, people became addicted to heroin in the 1960s or 1970s, you know, for them -- for many of them, government intervention in a drug epidemic remains synonymous with the war on drugs, which I know another caller brought up. You know, it's mandatory minimum prison sentences, no-knock search warrants. It's not public health outreach. It's not Naloxone.
JAMISONAnd in talking to people in other cities across the country that are experiencing similar locally based epidemics among their population of older African American heroin users, that seems to linger in many places. That there's a feeling that there's not -- that level of sympathy for drug users has not always reached this particular population. And for people like two of the people we wrote about in our stories and that my colleague Whitney Shefte did her excellent video of that that you played earlier on, Sam Rogers and Rene Howell, you know, these are people who have been using 30 years. And they say, well, this is terrific that we have this new outpouring of sympathy for drug users today. But, you know, where was this 20 or 30 years ago?
REEDWe've got a Tweet from Candace, who says, you can't talk about treating addiction without talking about mental health counseling. What will the district do to increase services in that area? Roger Mitchell, you're the District's chief medical examiner. What are you doing?
MITCHELLWell, I think that it's -- you know, I think it's important. There's no doubt that mental health and identifying with both acute stress and chronic stress of a community is extremely important in dealing with substance use disorder. Substance use disorder particular in this city is not one that is often tied up in the larger mental health-related issues like schizophrenia or schizoaffective disorder, but it is associated with depression and anxiety and functionally with access.
MITCHELLSo, I think that the District, as we're moving forward, has a plan that is being laid out surrounding not just treating the substance use disorder and MAT, but just as Dr. Chapman described, is ensuring that both MAT, medical assisted therapy for drug addiction, is coordinated with counseling. Because that's what you have to do in order to work through that, and then treating the whole patient. So, you can't just counsel them, either. You have to talk about what are the stressors that are getting them there. So, it's been said, access to housing, access to education, access to jobs. And so I think that this very ambitious strategic plan lays out some of those things that we are looking to be made accountable for.
CHAPMANI think in terms of the medical economics of psychiatry and psychology, because of the paucity of providers in the community, especially those that will accept Medicaid, that that becomes a major barrier. So, we're going to have to look at the economics of improving or increasing reimbursement where psychiatrists and psychologists can basically take cash only and totally ignore this particular population.
CHAPMANAnd one other barrier is just access, getting patients in the office, and then getting them the multiple services that they need. So we actually created what we call a virtual office using telemedicine, so that if we get a patient in the office and they need social service contact or if they need a psychiatrist, that without physically having them go to the psychiatrist or the psychiatrist come to them, that we can provide those types of services in a one-stop shop, which becomes very important because of the economic factors, travel, babysitting costs, etcetera, in this population.
REEDGot one last Tweet I can read on the air from HIPS, that's Helping Individual Prostitutes Survive. They've tweeted: D.C. Health has monthly Naloxone trainings, but the site is out of date. Unfortunately, that's all the time we have for today. Edwin Chapman is an internal medicine specialist in Washington, D.C. Thanks for being here.
CHAPMANThank you.
REEDDiane Jones is director of special programs and field education at Family Medical Counseling Services in D.C. Thanks for being here.
JONESThank you.
REEDRoger Mitchell is D.C.'s chief medical examiner. Thanks for being here.
MITCHELLThank you.
REEDAnd Peter Jamison's with the Washington Post. Thanks for being here.
JAMISONHappy to join you.
REEDToday's conversation on the local opioid crisis was produced by Julie Depenbrock. Again, if you have a story you'd like to share about how the shutdown has affected you, email us a 30-second voice memo at kojo@wamu.org. We'll play them on air. I'm Dan Reed, sitting in for Kojo Nnamdi.
On this last episode, we look back on 23 years of joyous, difficult and always informative conversation.
Kojo talks with author Briana Thomas about her book “Black Broadway In Washington D.C.,” and the District’s rich Black history.
Poet, essayist and editor Kevin Young is the second director of the Smithsonian's National Museum of African American History and Culture. He joins Kojo to talk about his vision for the museum and how it can help us make sense of this moment in history.
Ms. Woodruff joins us to talk about her successful career in broadcasting, how the field of journalism has changed over the decades and why she chose to make D.C. home.